
Self-expanding metallic stent placement for the palliation of malignant airway complications
Highlight box
Key findings
• Self-expanding metallic stents (SEMSs) using a flexible bronchoscope were effective in patients with severe emergent symptoms of tracheal malignant lesions, with a median overall survival of 75 days. Patients with symptomatic improvement after stent insertion had a relatively good prognosis, particularly when chemotherapy was administered after placing the stent.
What is known and what is new?
• Respiratory-esophageal fistula and respiratory stenosis are critical conditions, and the prognosis is poor when these conditions are not controlled.
• We report the most severe cases limited to tracheal lesions and using a flexible bronchoscope.
What is the implication, and what should change now?
• Tracheal lesions due to cancer cause critical condition and are associated with poor prognosis; however, early SEMS placement has been found to improve oxygenation and symptoms, enabling extubation even in patients receiving mechanical ventilator support.
• Placing SEMS via flexible bronchoscopy for appropriate cases enables early intervention, and it should be performed aggressively.
Introduction
Background
Tracheal stenosis and fistula are critical conditions that require early intervention. Malignant tumors, including lung cancer, metastatic tracheal tumors, and esophageal cancer, frequently result in tracheal stenosis or fistulas. Patients with tracheal stenosis or fistulas are at high risk when receiving general anesthesia because of pneumonia, dyspnea, and poor general condition. Stenting using a flexible bronchoscope can be performed under intravenous sedation. Self-expanding metallic stent (SEMS) insertion, rather than plastic tube insertion, is safer, more effective, and quicker in the palliation of dysphagia (1).
Severe stenosis (>50%) of the central airway and some degree of poor prognosis or tracheobronchial perforation are considered reasonable indications for airway stenting (2). In cancer-related strictures, airway stents can be used either for palliation to maintain airway patency after debulking or as a bridge to other procedures. The effectiveness of stenting has been reported in a retrospective analysis of 50 patients with advanced metastatic airway obstruction. In addition to providing excellent palliation, the timely placement of an expandable metal stent improves survival in patients with malignant stenosis (3).
Rationale and knowledge gap
Although there have been several studies of patients with airway stents inserted, standardizing the patient’s background is difficult. One reason for this is that the patient’s general condition and the need for emergency treatment may differ depending on the airway lesion’s location. Few reports exist on specific situations, including emergency cases or procedures limited to metallic stents using a flexible bronchoscope.
Objective
Herein, we describe the efficacy of tracheal stenting using a less invasive flexible bronchoscope for malignant tumors. We present this study in accordance with the STROBE reporting checklist (available at https://apm.amegroups.com/article/view/10.21037/apm-24-155/rc).
Methods
At Chiba University Hospital, we retrospectively reviewed the data of 13 patients who underwent tracheal SEMS placement for malignancy between January 2008 and December 2021. An Ultraflex stent (Boston Scientific, Marlborough, MA, USA) or an AERO stent (MERIT MEDICAL, Salt Lake City, UT, USA) was used. Overall, 76 tracheobronchial stents were placed in 63 patients, 25 of which were tracheal stents. Of these, 13 patients were included in the study, excluding five with implanted stents via rigid bronchoscopy and seven with spiral Z stents (Cook Inc., Bloomington, IN, USA), which are currently unavailable in Japan for safety reasons. The type of airway involvement was classified as external compression, invasive compression, fistula formation, or mixed (combination) (4). Tracheal stenosis was classified as extrinsic or intrinsic (endoluminal or submucosal). Technique-related complications were surveyed using medical records.
Symptom improvement was defined as decreased oxygen demand or improvement in subjective symptoms within 1 week of the procedure.
Ethical approval
The study was conducted following the tenets of the Declaration of Helsinki (as revised in 2013). The Institutional Review Board of Chiba University Graduate School of Medicine approved this study (approval number M10207), and individual consent for this retrospective analysis was waived.
Statistical analyses
Survival curves were obtained and compared using the Kaplan-Meier method and log-rank test, respectively. Statistical significance was set at P<0.05. Statistical analyses were performed using EZR (Saitama Medical Center, Jichi Medical University, Saitama, Japan).
Results
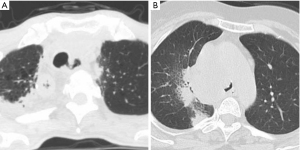
Baseline clinicopathological findings and outcomes of the 13 patients are summarized in Tables 1,2, respectively. The mean age of the patients was 68.7 (range, 60–82) years, and 11 patients were men (85%). All patients exhibited symptoms of central airway stenosis or fistulas. Tracheoesophageal fistula was diagnosed using esophagography, chest computed tomography (CT), and/or bronchoscopy. Typical CT findings are shown in Figure 1 (Cases 11 and 12 in Table 2). Figures 2,3 show the efficacy of metallic stents in managing tracheoesophageal fistulas (Case 6 in Table 2) and malignant intrinsic stenosis (Case 12 in Table 2), respectively.
Table 1
| Characteristics | Data (n=13) |
|---|---|
| Age (years) | 68.7±6.1 |
| Sex (male/female) | 11/2 |
| ECOG PS (0–1/2–4) | 5/8 |
| Fistula (yes/no) | 8/5 |
| Stenosis (<50%/≥50%) | 8/5 |
| Pre-stent therapy (yes/no) | 10/3 |
| AERO stent/Ultraflex stent | 2/11 |
| Technique-related complications (yes/no) | 1/12 |
| Symptom improvement (yes/no) | 10/3 |
| Post-stent therapy (yes/no) | 5/8 |
| OS (<90/≥90 days) | 7/6 |
Data are presented as mean ± SD or number. ECOG, Eastern Cooperative Oncology Group; OS, overall survival; PS, performance status; SD, standard deviation.
Table 2
| No. | Age (years) | Sex | Primary disease | ECOG PS | Pre-stent therapy | Symptom | Stenosis | Fistula | Complications | Symptom improvement | Post-stent therapy | Type of stents | Cause of death | D/A | OS (days) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 65 | M | Es | 4 | C, R | Dyspnea | – | Yes | Pneumonia exacerbation | – | – | Ultraflex | Pneumonia | D | 3 |
| 2 | 65 | F | Lu | 1 | S, R | Pneumonia → intubation | – | Yes | Trachea injury | – | – | AERO | Trachea injury | D | 3 |
| 3 | 82 | M | Es | 4 | C, R | Pneumonia | Ex | – | – | Yes | – | Ultraflex | Cancer | D | 8 |
| 4 | 66 | M | Es | 4 | C, R | Pneumonia | – | Yes | – | – | Ultraflex | – | A | 18 | |
| 5 | 77 | M | Es | 1 | – | Pneumonia/dysphagia | In | Yes | – | Yes | – | Ultraflex | Cancer | D | 22 |
| 6 | 62 | M | Es | 1 | C, R | Cough | – | Yes | Mediastinitis | Yes | – | Ultraflex | Unknown | D | 38 |
| 7 | 72 | M | Es | 3 | C | Dyspnea | In | – | – | Yes | C | Ultraflex | Cancer | D | 75 |
| 8 | 65 | M | Co | 2 | S, C | Dyspnea | In | – | Restenosis | Yes | C | Ultraflex | – | A | 98 |
| 9 | 72 | M | Es | 2 | C, R | Aspiration pneumonia | In | Yes | Hemorrhage | Yes | – | Ultraflex | Cancer | D | 107 |
| 10 | 74 | M | Es | 2 | – | Dyspnea | In | – | – | Yes | – | Ultraflex | Cancer | D | 109 |
| 11 | 60 | M | Es | 1 | C, S, R | Pneumonia | – | Yes | – | Yes | C | Ultraflex | – | A | 114 |
| 12 | 69 | F | Lu | 4 | – | Dyspnea →intubation | In | – | Atrial fibrillation | Yes | C | AERO | Cancer | D | 204 |
| 13 | 64 | M | Es | 1 | C, R | Aspiration pneumonia | – | Yes | – | Yes | C | Ultraflex | Cancer | D | 642 |
A, alive; C, chemotherapy; Co, colon cancer; D, dead; ECOG, Eastern Cooperative Oncology Group; Es, esophageal cancer; Ex, extrinsic; F, female; In, intrinsic; Lu, lung cancer; M, male; OS, overall survival; PS, performance status; R, radiotherapy; S, surgery.


Pathologic diagnosis was esophageal cancer in 10 patients, lung cancer in two, and colon cancer in one. Pneumonia due to trachea-esophageal fistula and dyspnea caused by stenosis were common indications in this cohort, and 2 (15.4%) patients required intubation and mechanical ventilation for respiratory management before stent insertion. Ten (76.9%) patients underwent therapeutic intervention before stenting, including surgery, chemotherapy, radiation therapy, or a combination of these interventions. Nine (69.2%) patients had fistulas, and six of them had accompanying stenosis. Six of these cases had fistulas due to the effects of treatment. Seven (53.8%) patients had stenosis, of whom one and six had tracheal extrinsic stenosis and intrinsic stenosis, respectively. Severe stenosis, defined as more than 50% of the inner cavity, was observed in 6 patients (46.2%), and two of them showed hazardous stenoses at over 90%. In four patients, the procedures were performed in the operating room under general anesthesia using propofol and muscle relaxants. However, in nine patients, the procedures were performed in the endoscopy room using sedation with midazolam under spontaneous breathing.
Ultraflex/AERO stents were used in 11/2 patients; the location was the trachea in 11 patients and both the trachea and bronchus in two. Complications related to the procedure were observed in 7 patients (53.8%) as follows: one, membranous trachea injury; one, hemoptysis; two, pneumonia without improvement; one, mediastinitis; and two, restenosis, although no stent migration was observed. The mean time from the decision of stent indication to insertion was 3.6 (range, 0–11) days. Five (38.4%) patients were discharged home, 5 (38.4%) were transferred to another hospital, and the other three died in the hospital without discharge or transfer. All transfer cases were for rehabilitation and recovery. Despite some cases showing an unknown prognosis with poor performance status (PS) after the transfer (Case 4 in Table 2), 50% (3/6) of the transferred patients who demonstrated improved PS after stenting survived for more than 3 months.
After stenting, 3 (23.1%) patients showed disease exacerbation without symptomatic improvement, and 5 (38.4%) demonstrated subjective improvement. The remaining 5 (38.4%) patients had improved symptoms and clinical findings: mechanical ventilation was ceased in two patients, and oxygen supplementation could be reduced in the remaining three after stenting. Six (46.2%) patients received additional chemotherapy for malignancy. The median survival time of all patients was 75 days, although 5 (38.5%) died within 30 days. Patients who achieved symptomatic improvement (n=10) after the procedure had a better prognosis than those who did not (107 vs. 3 days, P=0.02; Figure 4A). Furthermore, patients who could be treated with additional chemotherapy (n=5) showed the same tendency (204 vs. 22 days, P=0.01; Figure 4B).

Discussion
Key findings
Interventional bronchoscopy with stenting has been proven to be an effective treatment for malignant airway lesions (2,3,5,6). The advantage of SEMS placement is that it can be performed if the patient is already intubated because of respiratory failure or without general anesthesia. In this study, the target cohort comprised patients with tracheal emergencies due to malignancy, and a metallic stent was inserted using a flexible bronchoscope. In this cohort, tracheal stents were frequently referred for tracheoesophageal fistula, pneumonia, or severe stenosis due to esophageal cancer, and many were for lifesaving purposes or palliation. In two patients, the stent was placed during intubation, enabling extubation and demonstrating its effectiveness. Six (42.9%) patients showed improvement in symptoms, which enabled additional treatment and prolonged survival.
All cases were in critical condition, and without treatment, it appeared their PS would rapidly deteriorate, with a prognosis of a few days to a few weeks. Case 12 in Table 2 survived for more than 6 months after stenting. It could be certain that some populations receive great benefits from SEMS regarding prognosis. Furthermore, our analysis revealed no significant difference in prognosis between the two groups with pretreatment Eastern Cooperative Oncology Group (ECOG) PS scores of 0–1 and 2–4 (P=0.66). We also compared whether the onset of disease was due to treatment (n=6) or disease progression (n=7); however, no difference was found in prognosis in this cohort (P=0.64). ECOG PS score and disease progression before stent insertion did not influence prognosis.
Strengths and limitations
Both silicone and metallic stents can be used in airway emergencies due to malignancy. The placement of a silicone Y-stent is a safe and effective procedure, as shown by a systematic review that yielded nine studies on airway obstruction or tracheoesophageal fistula (7,8). Metallic and silicone stents were equally successful and safe, and no significant differences were found when mortality was considered in the competitive risk analysis (9,10). However, one disadvantage of inserting silicone stents is that a rigid bronchoscopy is required for the procedure. This indicates a risk of general anesthesia and difficulty in patients who have already been intubated. In some specific cases, rigid bronchoscopy is preferable, such as when coring out a tumor or when bleeding control is required. Generally, using only flexible bronchoscopy is easy and preferable for patients with poor PS, and the procedure is simple and less invasive. In this cohort, using metal stents without a rigid speculum and focusing only on tracheal lesions allowed us to concentrate on severe cases with low PS, and we could demonstrate efficacy in these cases. Regarding the limitation, the small number of patients at a single center was insufficient to discuss the type of stent and patient prognosis, and the prognoses of some patients were unknown because they were transferred to other hospitals. Additionally, four cases where general anesthesia was used to perform stent insertion were included. This was because when an operating room was available, we performed the procedure there since it would enable a quicker response in case of any sudden changes in the patient’s condition. When an operating room was used, minimal required general sedation was applied because an anesthesiologist was responsible for circulation and respiratory management at Chiba University Hospital. Thus, we considered that operating room use or general anesthesia did not affect disease severity or prognosis but contributed to patient respiratory distress relief.
Comparison with similar research
The prognosis for successful stenting of an airway esophageal fistula is approximately 3 months, compared to that for an uncontrolled fistula, which is a few weeks (9,11). The prognosis after stenting was worse with fistulas (11,12). However, no prognostic difference was found between patients with and those without fistulas in this study. Early stent insertion and secure fistula closure were the most critical issues addressed in this study, and it is easy to assume that stent insertion can reduce distress in these patients. Takigawa et al. indicated the effectiveness of placing the AERO stent in patients with poor PS (grades 3–4), including those intubated (13). Approximately 80% of patients showed improved dyspnea, PS, and symptoms after SEMS implantation, which is similar to the findings of our study (12,14).
In this study, patients whose subjective or clinical symptoms improved after the procedure had a significantly better prognosis (P=0.02). Furthermore, patients who received chemotherapy after stenting had a significantly better prognosis (P=0.01), a result similar to that observed in a previous study on the efficacy of airway stents for esophageal cancer (11,12). Accordingly, patients whose general condition deteriorated due to pneumonia or dyspnea were also considered good candidates for this treatment if their symptoms were expected to improve and additional treatment options were available.
Explanations of findings
The European Society of Gastrointestinal Endoscopy, in its 2021 publication, recommends esophageal SEMS placement to seal malignant tracheoesophageal or bronchoesophageal fistulas (strong recommendation, low-quality evidence). It also recommends double-stent placement (esophagus and airway) when fistula occlusion is not achieved by a single stent (strong recommendation, low-quality evidence) (8,13). In this study, metallic stents were implanted in patients with tracheoesophageal fistula or stenosis due to esophageal cancer, and they were approached using flexible bronchoscopy alone. No adverse events, such as esophageal stenosis and dysphagia, were observed. However, only two patients showed exacerbation of pneumonia due to failure of complete closure of the fistula and a massive tracheoesophageal fistula caused by tracheal injury, which might have been indications for double stenting. Herth et al. reported that the survival rate of the airway stent group was significantly lower than that of the esophageal and double-stent groups; however, the reason for this remains unclear and may be because patients in the airway stent group had more advanced disease (10). Airway stents alone may be considered effective if appropriate cases, such as those with mild esophageal stenosis, are selected.
Implications and actions needed
Cases with tracheal stent insertion frequently vary widely in terms of urgency and severity, making it difficult to distinguish between palliative procedures and those undergoing treatment for cancer. Future studies with more cases from multiple centers and those that matched patient backgrounds through specific patient selection are desirable.
Conclusions
Minimally invasive tracheal stent insertion using a flexible bronchoscope for tracheal lesions was effective with or without PS of patients or therapeutic intervention before stent insertion. Patients with symptomatic improvement after stent insertion had a relatively good prognosis, particularly when chemotherapy was administered after placing the stent.
Acknowledgments
None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://apm.amegroups.com/article/view/10.21037/apm-24-155/rc
Data Sharing Statement: Available at https://apm.amegroups.com/article/view/10.21037/apm-24-155/dss
Peer Review File: Available at https://apm.amegroups.com/article/view/10.21037/apm-24-155/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://apm.amegroups.com/article/view/10.21037/apm-24-155/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the tenets of the Declaration of Helsinki (as revised in 2013). The study was approved by the ethics committee of Chiba University Graduate School of Medicine (approval number M10207), and individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Dai Y, Li C, Xie Y, et al. Interventions for dysphagia in oesophageal cancer. Cochrane Database Syst Rev 2014;2014:CD005048. [Crossref] [PubMed]
- Ost DE, Ernst A, Grosu HB, et al. Therapeutic bronchoscopy for malignant central airway obstruction: success rates and impact on dyspnea and quality of life. Chest 2015;147:1282-98. [Crossref] [PubMed]
- Razi SS, Lebovics RS, Schwartz G, et al. Timely airway stenting improves survival in patients with malignant central airway obstruction. Ann Thorac Surg 2010;90:1088-93. [Crossref] [PubMed]
- Chhajed PN, Somandin S, Baty F, et al. Therapeutic bronchoscopy for malignant airway stenoses: choice of modality and survival. J Cancer Res Ther 2010;6:204-9. [Crossref] [PubMed]
- Chung FT, Lin HC, Chou CL, et al. Airway ultraflex stenting in esophageal cancer with esophagorespiratory fistula. Am J Med Sci 2012;344:105-9. [Crossref] [PubMed]
- Murthy S, Gonzalez-Stawinski GV, Rozas MS, et al. Palliation of malignant aerodigestive fistulae with self-expanding metallic stents. Dis Esophagus 2007;20:386-9. [Crossref] [PubMed]
- Sehgal IS, Dhooria S, Madan K, et al. Placement of tracheobronchial silicone Y-stents: Multicenter experience and systematic review of the literature. Lung India 2017;34:311-7. [Crossref] [PubMed]
- Spaander MCW, van der Bogt RD, Baron TH, et al. Esophageal stenting for benign and malignant disease: European Society of Gastrointestinal Endoscopy (ESGE) Guideline - Update 2021. Endoscopy 2021;53:751-62. [Crossref] [PubMed]
- Ortiz-Comino RM, Morales A, López-Lisbona R, et al. Silicone Stent Versus Fully Covered Metallic Stent in Malignant Central Airway Stenosis. Ann Thorac Surg 2021;111:283-9. [Crossref] [PubMed]
- Herth FJ, Peter S, Baty F, et al. Combined airway and oesophageal stenting in malignant airway-oesophageal fistulas: a prospective study. Eur Respir J 2010;36:1370-4. [Crossref] [PubMed]
- Wang H, Ke M, Li W, et al. Chinese expert consensus on diagnosis and management of acquired respiratory-digestive tract fistulas. Thorac Cancer 2018;9:1544-55. [Crossref] [PubMed]
- Cheng WC, Shen MF, Wu BR, et al. The prognostic predictors of patients with airway involvement due to advanced esophageal cancer after metallic airway stenting using flexible bronchoscopy. J Thorac Dis 2019;11:3929-40. [Crossref] [PubMed]
- Takigawa Y, Sato K, Kudo K, et al. Effectiveness of AERO Stent Placement for Malignant Airway Disorder in Patients with a Poor Performance Status. Intern Med 2024;63:2277-82. [Crossref] [PubMed]
- Usuda K, Iwai S, Yamagata A, et al. Clinical outcomes and survival following placement of self-expandable metallic stents for central airway stenosis and fistula. Thorac Cancer 2021;12:48-56. [Crossref] [PubMed]


